Verify Insurance Before Treatment Avoid Claim Denials
Ensure every patient’s coverage is confirmed before services are delivered. Our expert eligibility verification team helps you reduce billing errors, prevent claim rejections, and improve your revenue cycle efficiency.
Our Eligibility Verification Services Include
We offer accurate and efficient eligibility verification to ensure patients’ insurance coverage is confirmed before services are provided. This helps reduce claim denials, minimize billing errors, and improve overall reimbursement success rates.
Insurance Eligibility Verification
We confirm whether a patient’s insurance plan is active and covers the scheduled services.
Copay & Deductible Verification
Accurate identification of patient financial responsibility, including copays, coinsurance, and deductibles.
Prior Authorization Verification
We ensure required authorizations are obtained in advance to prevent claim rejections.
Benefits Verification
Detailed breakdown of covered services, limitations, and exclusions to avoid surprises during billing.

Insurance Eligibility Verification
Ensure Accurate Coverage Before Every Visit
Our streamlined process ensures accuracy and efficiency
- Collect patient insurance information
- Verify eligibility with insurance providers
- Confirm benefits and coverage details
- Identify copays and deductibles
- Check prior authorization requirements
- Update records and notify provider
Our Eligibility Verification Services Include
Our Eligibility Verification Services ensure that patient insurance details are accurately confirmed before treatment. We verify coverage, benefits, copays, and prior authorizations to minimize claim denials. This helps healthcare providers streamline billing and improve reimbursement rates.
Step-by-Step Insurance Eligibility Verification Process
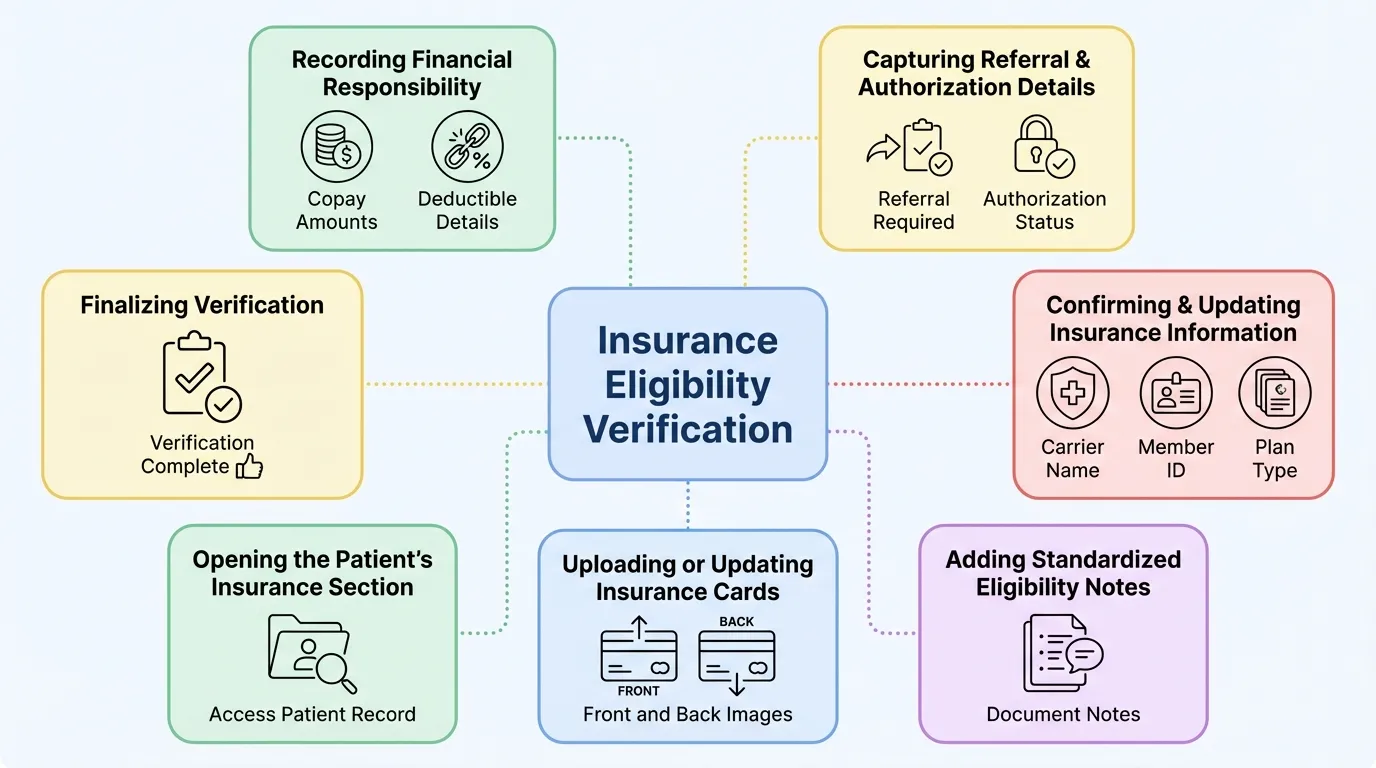
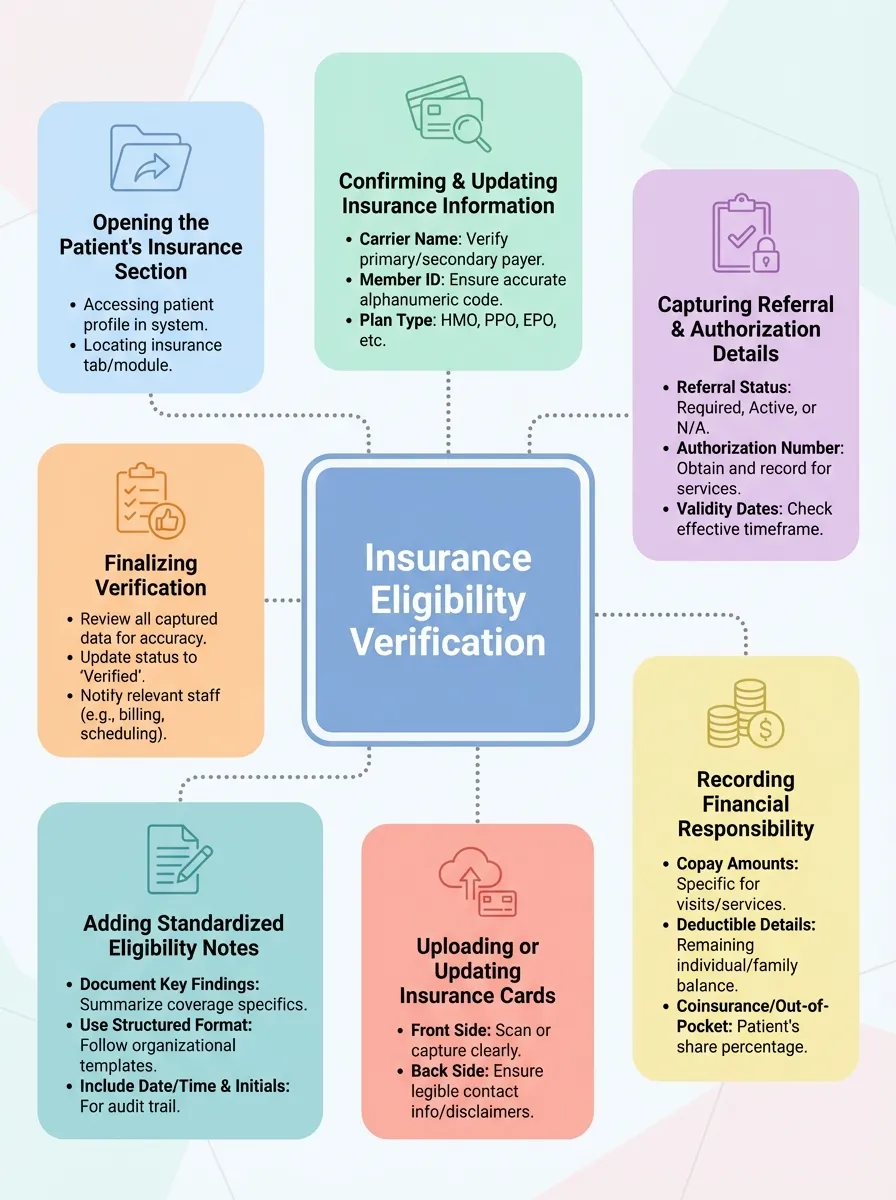
Common Issues We Solve Problems We Help You Prevent
We address the most frequent challenges that disrupt your revenue cycle and lead to financial losses. Our eligibility verification process helps prevent issues like incorrect patient information, inactive insurance coverage, and missing prior authorizations.
Inactive Coverage
We catch inactive or lapsed insurance before services are rendered, preventing denied claims.
Incorrect Benefit Details
We verify exact benefit details to eliminate billing disputes and patient confusion.
Missing Prior Authorizations
We confirm all required authorizations before services are delivered to prevent rejections.
Patient Cost Unclear
We provide patients with accurate cost estimates upfront to improve collections.
Frequently Asked Questions (FAQs)
It is the process of confirming a patient’s insurance coverage and benefits before providing medical services.
It prevents claim denials, ensures accurate billing, and improves revenue cycle efficiency.
Yes, we verify all patient financial responsibilities in advance.
It is approval from the insurance company required before certain services are performed.
We provide fast and efficient verification to support smooth patient workflows.
Reduce Claim Denials & Increase Your Healthcare Revenue
Claim denials can significantly impact your practice’s revenue and cash flow. At Nobel Healthcare RCM, we minimize errors in billing and coding through accurate processes and strict compliance with payer guidelines. Our expert team ensures clean claim submissions, faster approvals, and efficient follow-ups—helping you boost reimbursements and maintain a steady revenue stream.
