Maximize Revenue with Expert Denial & Rejection Management
Our Denial & Rejection Management services help reduce revenue loss by quickly identifying, correcting, and resubmitting denied claims. We improve approval rates and ensure faster reimbursements for better cash flow.
Reduce Revenue Loss with Proactive Denial Management
Denied and rejected claims can significantly impact your revenue cycle if not managed efficiently. Studies show that a large percentage of denied claims are never reworked, leading to permanent revenue loss. Our expert team ensures every claim is reviewed, corrected, and resubmitted promptly to maximize reimbursements.
Faster claim reprocessing
We quickly correct and resubmit denied claims to avoid payment delays.
Reduced denial rates
Our proactive approach minimizes errors and prevents future denials
Improved first-pass acceptance rate
Clean and accurate claims increase approvals on the first submission.
Accurate root cause analysis
We identify the exact reasons for denials to fix issues at the source.
Dedicated follow-up team
Our specialists consistently track and follow up on all denied claims.
Compliance with payer guidelines
We ensure every claim meets insurance requirements to avoid rejections.
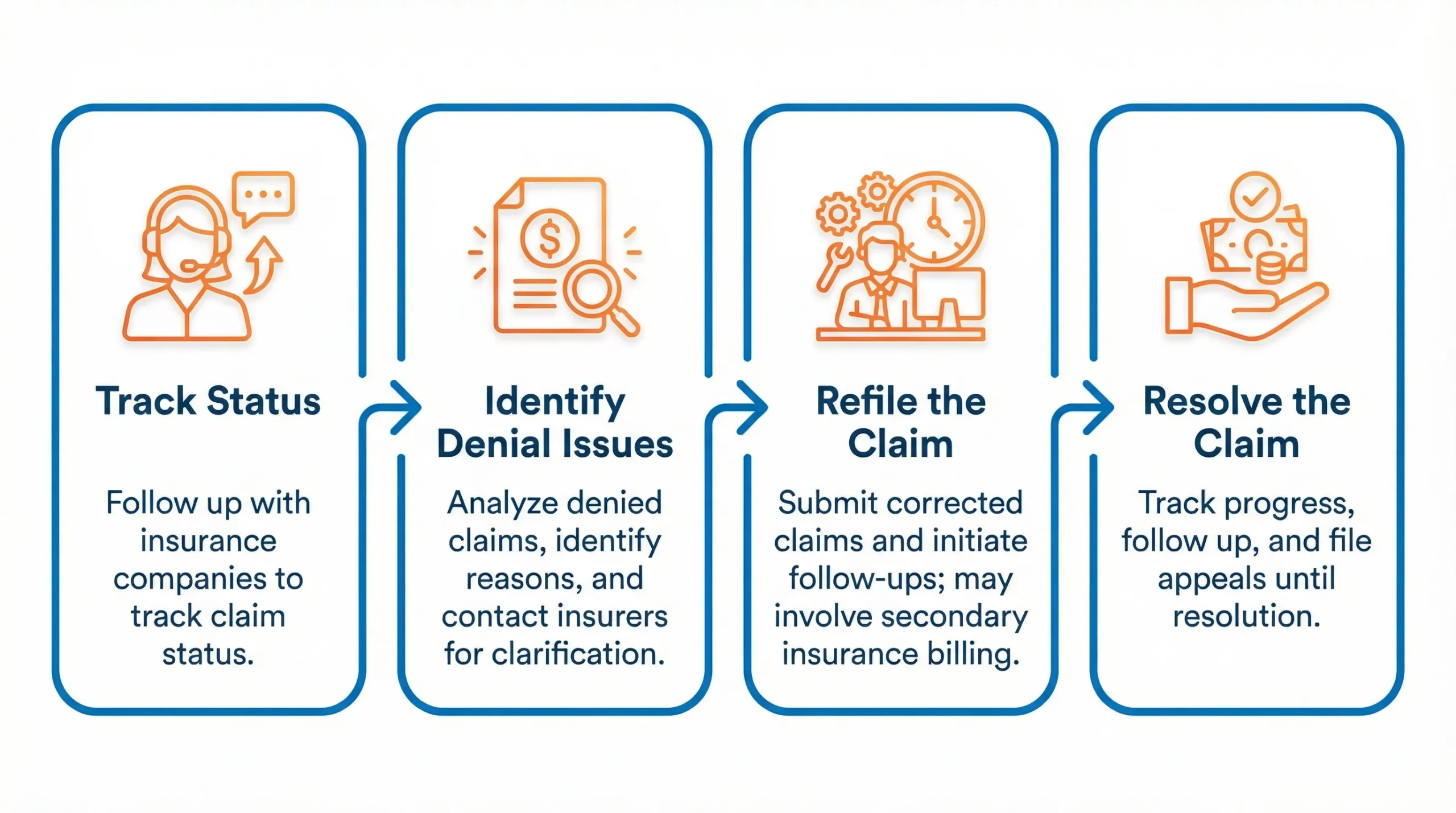
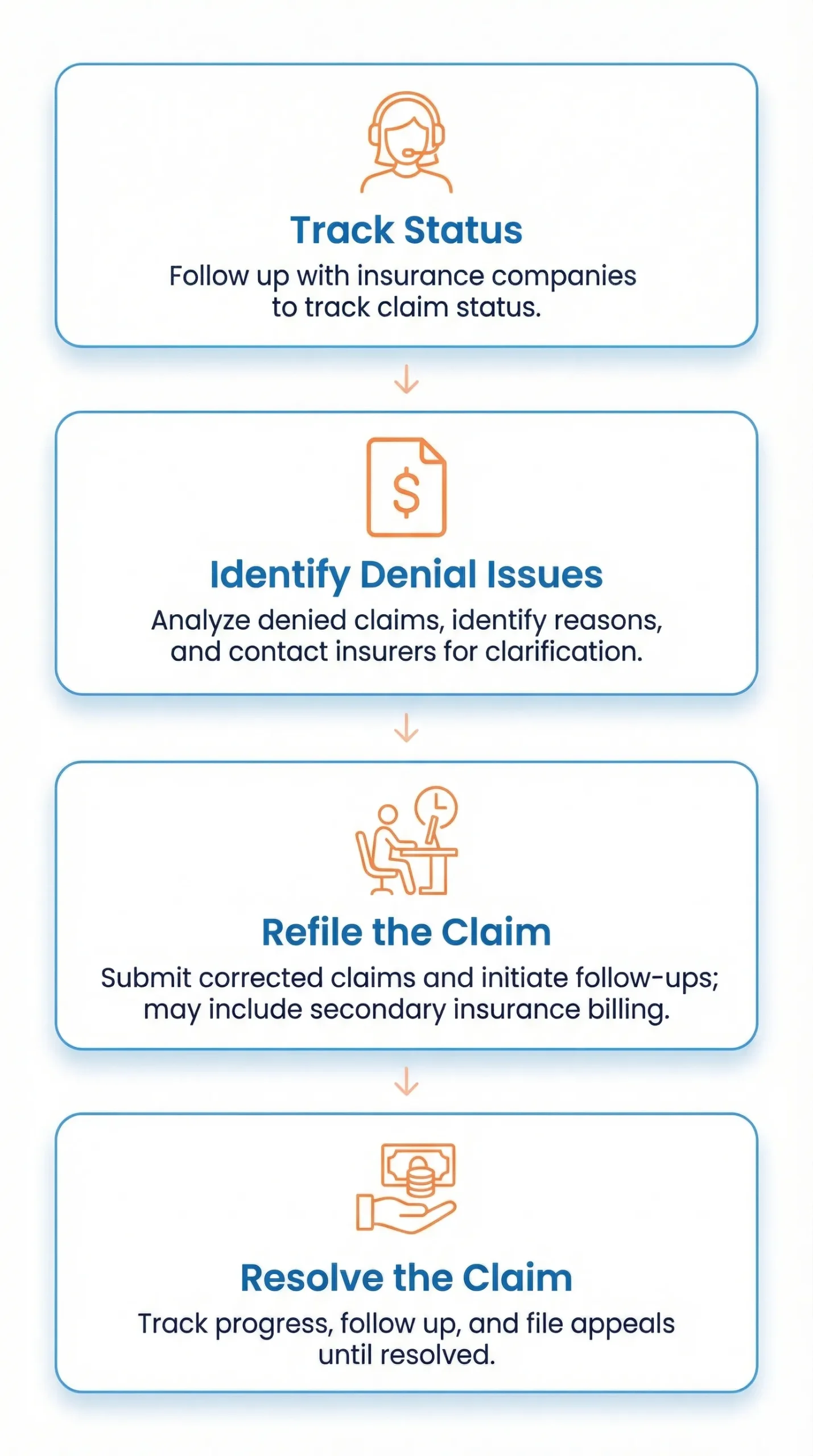
Step-by-Step Insurance Eligibility Verification Process
Why Choose Us
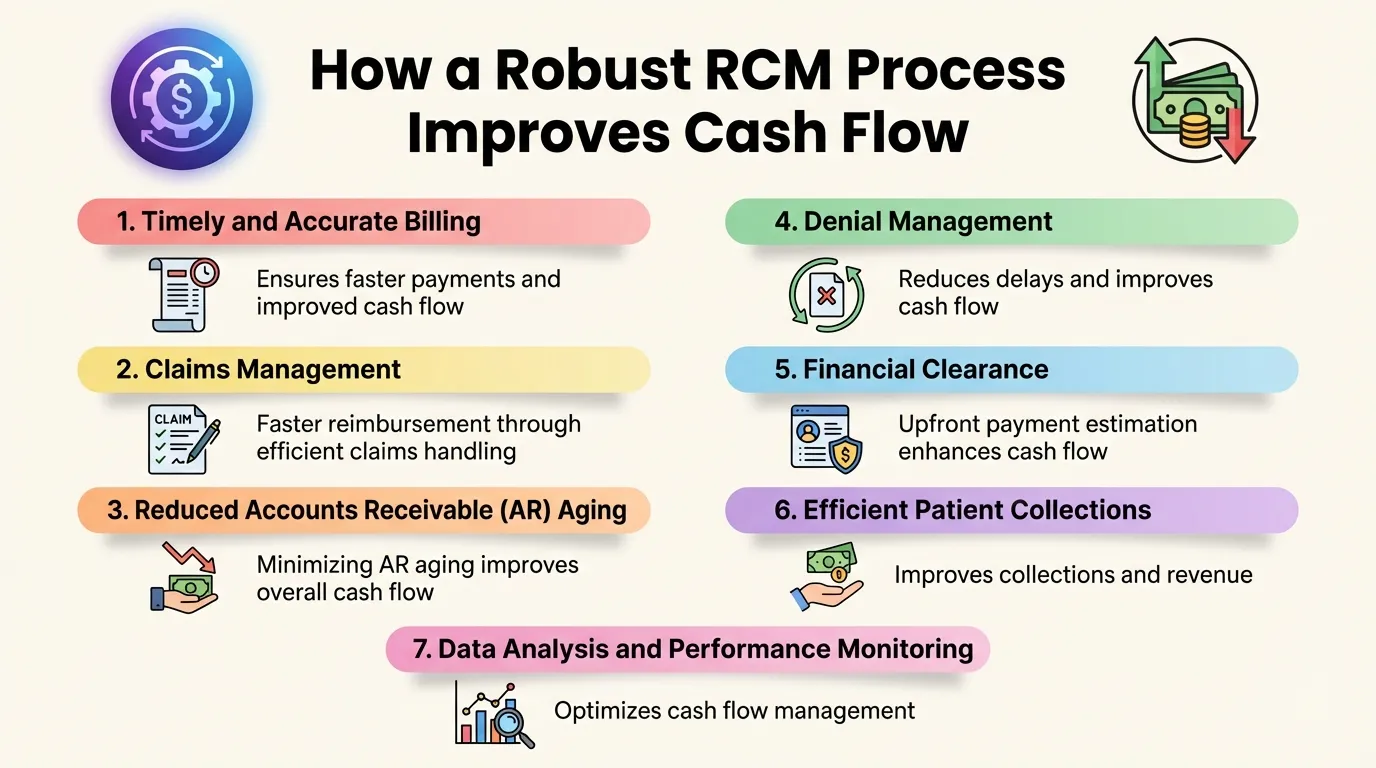
We provide reliable, results-driven denial management solutions designed to recover lost revenue and strengthen your revenue cycle. Our expert team combines industry knowledge, advanced technology, and proven strategies to ensure maximum claim recovery with complete transparency and compliance.

Frequently Asked Questions (FAQs)
Denial management is the process of identifying, analyzing, correcting, and resubmitting denied or rejected insurance claims to recover revenue.
A rejection occurs before claim processing due to errors, while a denial happens after the claim is reviewed but not approved for payment.
Common reasons include incorrect coding, missing information, eligibility issues, or lack of medical necessity.
Yes, most denied claims can be corrected and resubmitted or appealed successfully if handled properly.
It depends on the payer, but timely follow-ups can significantly speed up the process.
By reducing claim loss, increasing approval rates, and ensuring faster reimbursements.
Reduce Claim Denials & Increase Your Healthcare Revenue
Claim denials can significantly impact your practice’s revenue and cash flow. At Nobel Healthcare RCM, we minimize errors in billing and coding through accurate processes and strict compliance with payer guidelines. Our expert team ensures clean claim submissions, faster approvals, and efficient follow-ups—helping you boost reimbursements and maintain a steady revenue stream.
