Revenue Cycle Management (RCM) Services
Streamline your entire billing process, reduce denials, and maximize revenue with our comprehensive RCM solutions.

Why Choose Us
What is Revenue Cycle Management (RCM)?
Revenue Cycle Management (RCM) is the complete financial process that healthcare providers use to manage patient revenue—from initial appointment scheduling and patient registration to final payment collection. An efficient RCM system ensures accurate billing, timely reimbursements, and minimal claim denials. Our RCM services are designed to optimize every stage of your revenue cycle, helping your practice achieve consistent financial growth.
Why Choose Our RCM Services?
- Experienced RCM Professionals
- End-to-End Solutions
- Advanced Technology
- High Accuracy Rate
- List Item
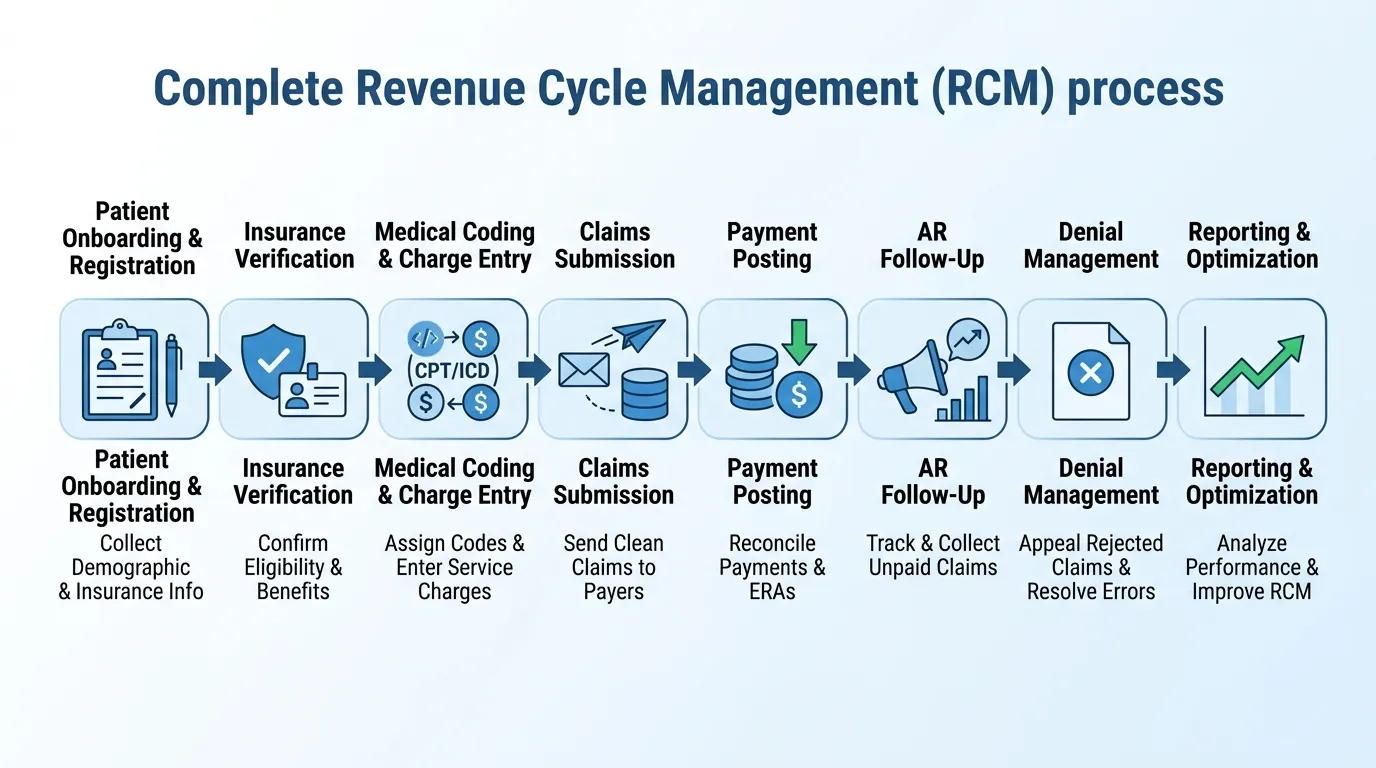
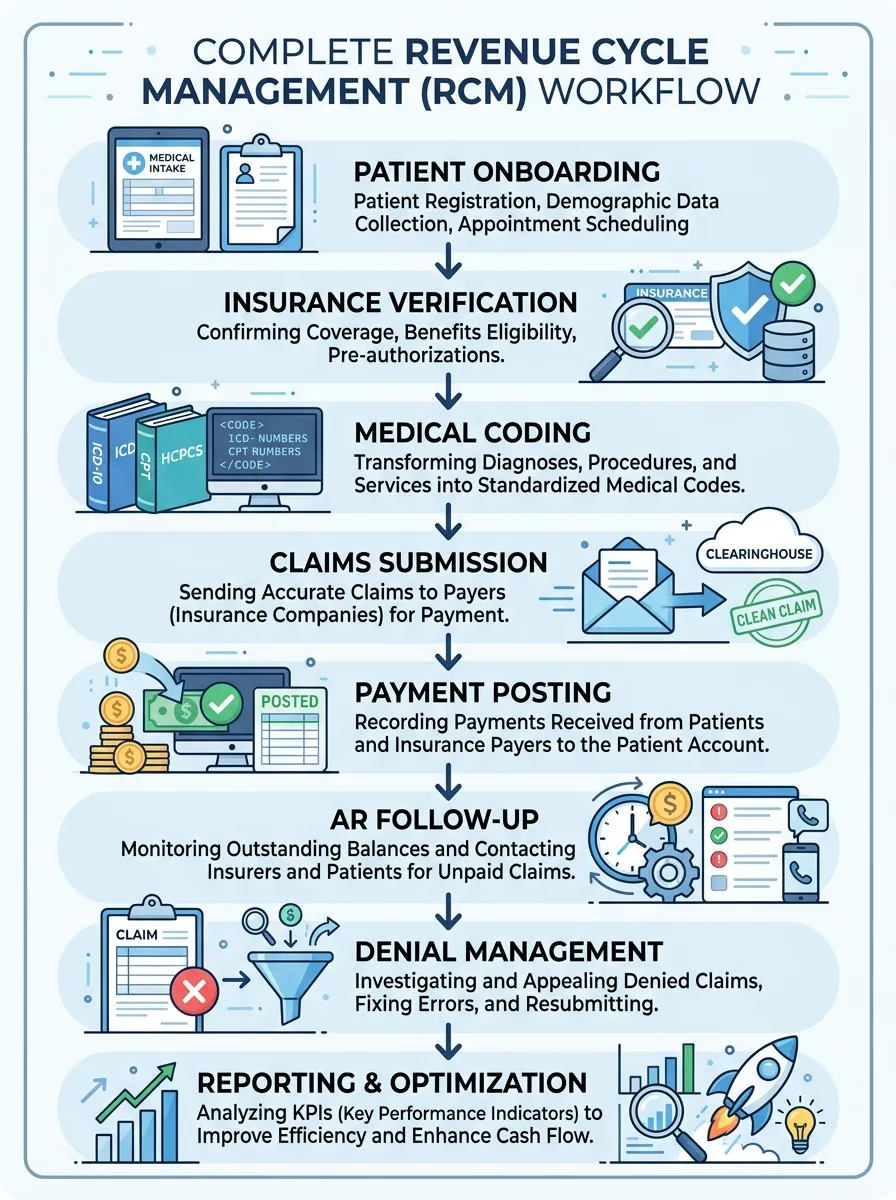
Comprehensive Revenue Cycle Management Services
Patient Registration
Insurance Check
Medical Coding
Claims Submission
Payment Posting
AR Follow-Up
Denial Management
Financial Reporting
Why Nobel Healthcare RCM
Why Choose Our RCM Services?
We deliver accurate, secure, and end-to-end revenue cycle solutions using expert professionals and advanced technology to maximize your practice revenue.
End-to-End Solutions
Experienced RCM Professionals
Advanced Technology
High Accuracy Rate
HIPAA-Compliant Process

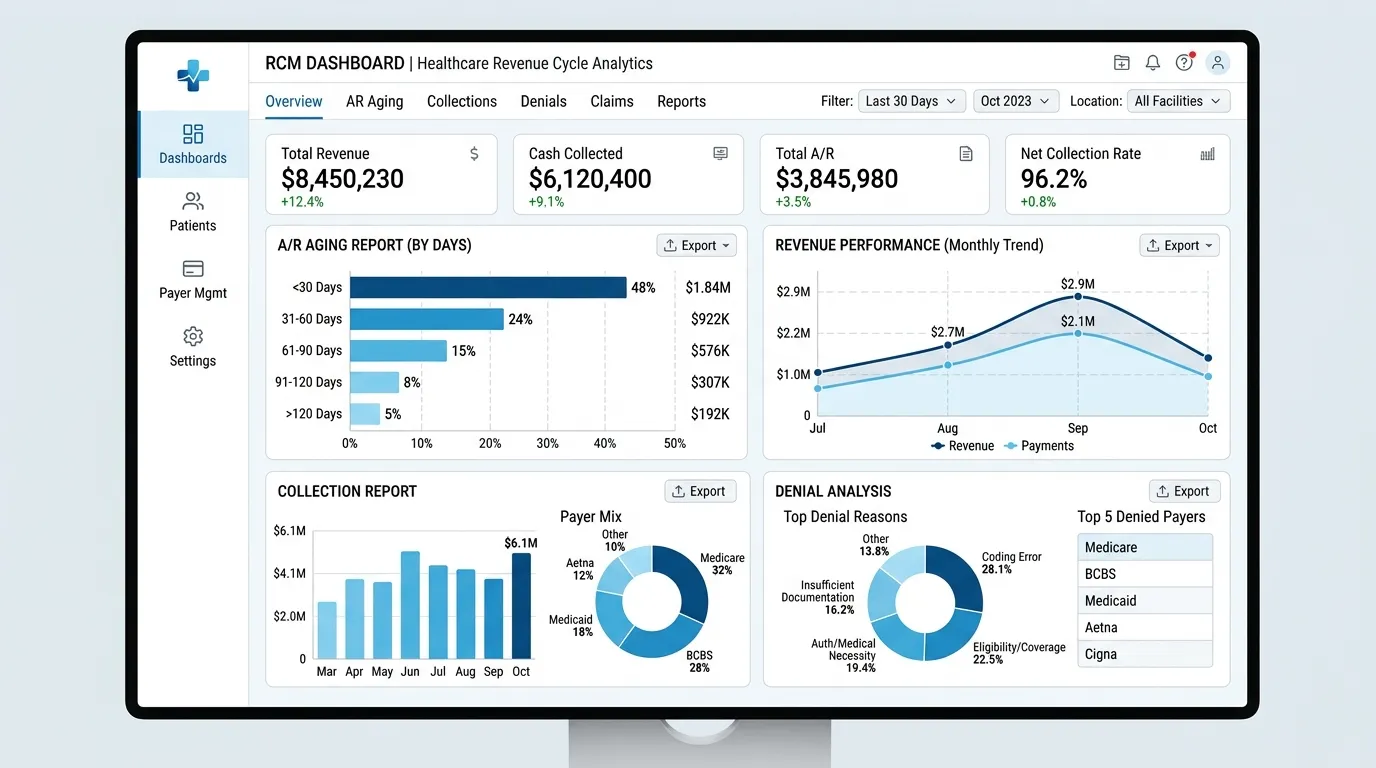
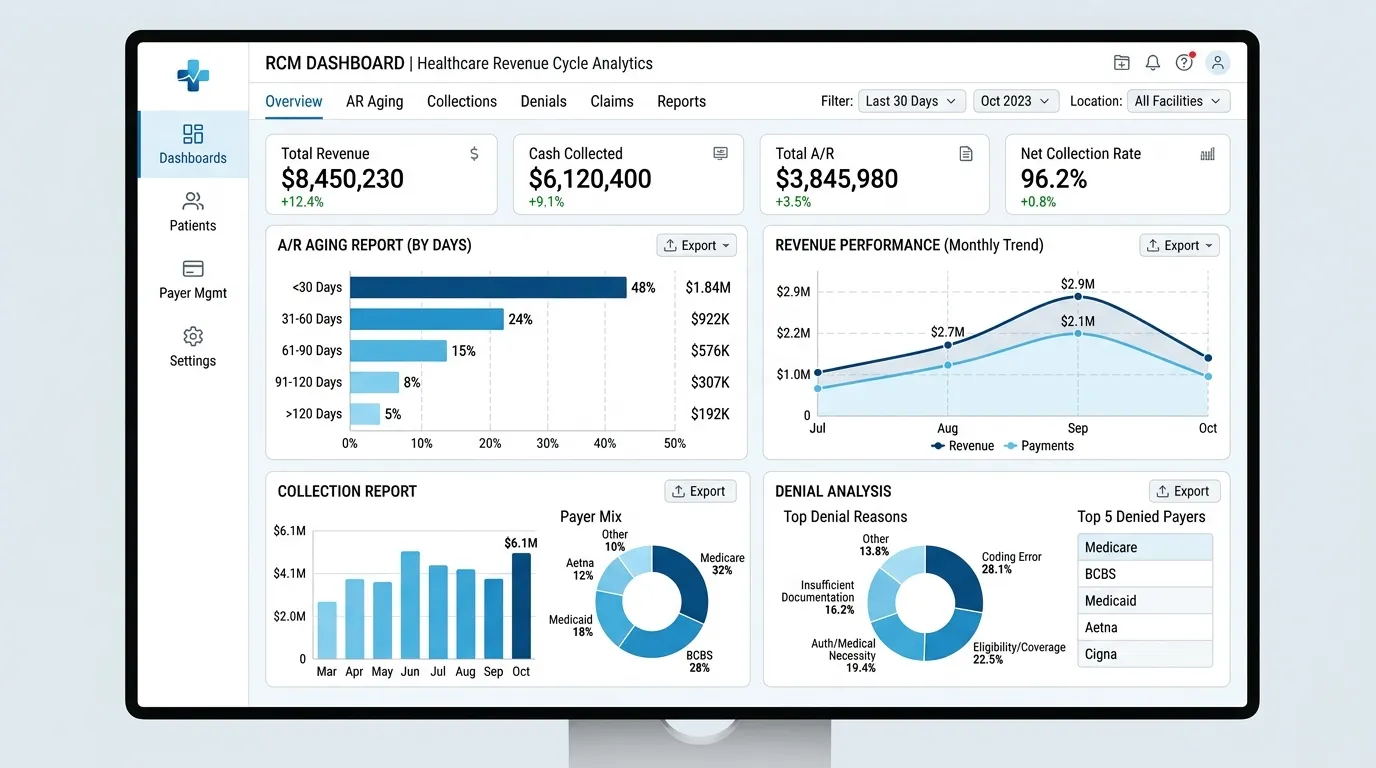
Revenue Performance Dashboards
Frequently Asked Questions (FAQs)
It is the process of confirming a patient’s insurance coverage and benefits before providing medical services.
It prevents claim denials, ensures accurate billing, and improves revenue cycle efficiency.
Yes, we verify all patient financial responsibilities in advance.
It is approval from the insurance company required before certain services are performed.
We provide fast and efficient verification to support smooth patient workflows.
Reduce Claim Denials & Increase Your Healthcare Revenue
Claim denials can significantly impact your practice’s revenue and cash flow. At Nobel Healthcare RCM, we minimize errors in billing and coding through accurate processes and strict compliance with payer guidelines. Our expert team ensures clean claim submissions, faster approvals, and efficient follow-ups—helping you boost reimbursements and maintain a steady revenue stream.
